Overview:
So, why are we including information about these important medical disorders on this, a dental website? There are two important reasons. First, it is very possible that your dental health or the longevity of your dental treatment may be affected by these disorders. Second, special appliances that can only be made and placed by dentists are becoming increasingly important tools in their management. We believe that it is time for dentistry to assume its role in managing these disorders – for our patients’ dental health as well as their overall wellbeing.
Sleep quality affects both your physical and mental performance during waking hours, as well as your overall health and quality of life. Three of the most important and common sleep disorders include snoring, obstructive sleep apnea, and nocturnal parafunction (or nocturnal bruxism). To begin understanding these disorders, it is important to distinguish snoring from obstructive sleep apnea.
Snoring is a relatively harmless, although annoying, activity that affects about one half of all adults to some degree. It is the harsh sound that occurs when your breathing is partially obstructed in some way while you sleep. Simple snoring results in little more than noise (and a resultant unhappy bed partner) and perhaps some restless sleep. However, between 10% and 25% of habitual snorers also have obstructive sleep apnea. It is for this reason that if you are being treated for snoring, it is important to first determine if you might also have sleep apnea (see “Testing and Evaluating” below).
Unlike snoring, obstructive sleep apnea is a potentially life threatening condition that affects between 3% and 7% of the adult population. It is a serious sleep disorder in which breathing repeatedly stops and restarts during sleep. Most patients with obstructive sleep apnea don’t even know they have it. It is estimated that less than 10% of those suffering from obstructive sleep apnea actually know they have the condition and seek help. Most believe they have a harmless snoring issue, as 70% to 95% of patients suffering from obstructive sleep apnea also snore
Nocturnal parafunction involves the involuntary activity of jaw muscles during sleep and includes the grinding (bruxing) or squeezing (clenching) of teeth during sleep. Unfortunately, past methods of measuring the incidence of these activities were based on unreliable questionnaires filled out by patients. Therefore, there are currently no accurate estimates of how many people actually suffer from these issues. However, it is safe to say that they affect a very large percent of the population (male and female, young and old) and are influenced by a wide variety of factors. They can result in damage to any part of the jaw system (teeth, jaw muscles, jaw joints, and periodontium) as well as other structures in the head and neck.
Signs, Symptoms, and Problems:
The following are common signs, symptoms, and problems associated with these disorders. While each disorder is listed separately, it is important to understand that it is common or even typical for any given patient to be affected by more than one of them.
Signs and symptoms of obstructive sleep apnea include:
- Waking up with a very sore or dry throat,
- Loud snoring,
- Occasionally waking up with a choking or gasping sensation,
- Sleepiness or lack of energy during the day,
- Sleepiness while driving,
- Morning headaches
- Restless sleep, and
- Forgetfulness, mood changes, and a decreased interest in sex.
Life threatening diseases or conditions affected by obstructive sleep apnea include:
- High blood pressure,
- Heart disease,
- Stroke,
- Automobile accidents caused by falling asleep at the wheel,
- Diabetes, and
- Depression.
Problems within the jaw system caused by nocturnal parafunction include:
- Worn, broken, loose, or sensitive teeth,
- Receding gums
- Damaged dental work,
- Damaged jaw joints (TMJ’s or Temporomandibular joints),
- Jaw pain,
- Headaches, and
- “TMD” symptoms.
Testing and Evaluation:
Because of the seriousness of obstructive sleep apnea, accurate testing and evaluation are critical and should be performed before treating either obstructive sleep apnea or snoring. This has traditionally been achieved with a supervised sleep study in a medical sleep center. In this type of study, the patient is connected to a monitor that records many sleep activities in a hospital room-like environment outside their home. In cases where unusual or complex sleep disorders exist, this type of study is still necessary. However, many patients feel that information gathered in these studies does not always represent their real life sleep performance – in their own home and bed, without someone observing them. In addition, such studies are expensive and record additional information that is not needed to diagnose obstructive sleep apnea (or snoring or nocturnal parafunction).
For these reasons, monitors for home sleep studies have been developed. These units range in capability from simply recording snoring activity to gathering all the information needed to determine your obstructive sleep apnea status. One such home sleep monitor is the NOX T-3 Sleep/Bruxism monitor by DDME. Not only does this system accurately record all the information needed to diagnose obstructive sleep apnea (as well as snoring and nocturnal parafunction), but this information can quickly (in less than 24hr.) and inexpensively be transmitted to and interpreted by a board certified sleep physician for evaluation and diagnosis. This type of physician diagnosis and evaluation guides appropriate treatment and is legally necessary in order for a dentist to provide treatment for obstructive sleep apnea (it also helps patients attain medical insurance reimbursement). The convenience, ease, and safety of the DDME system cannot be overstated. It is for this reason that we have incorporated this technology and this system into our office.
The NOX T-3 Monitor:
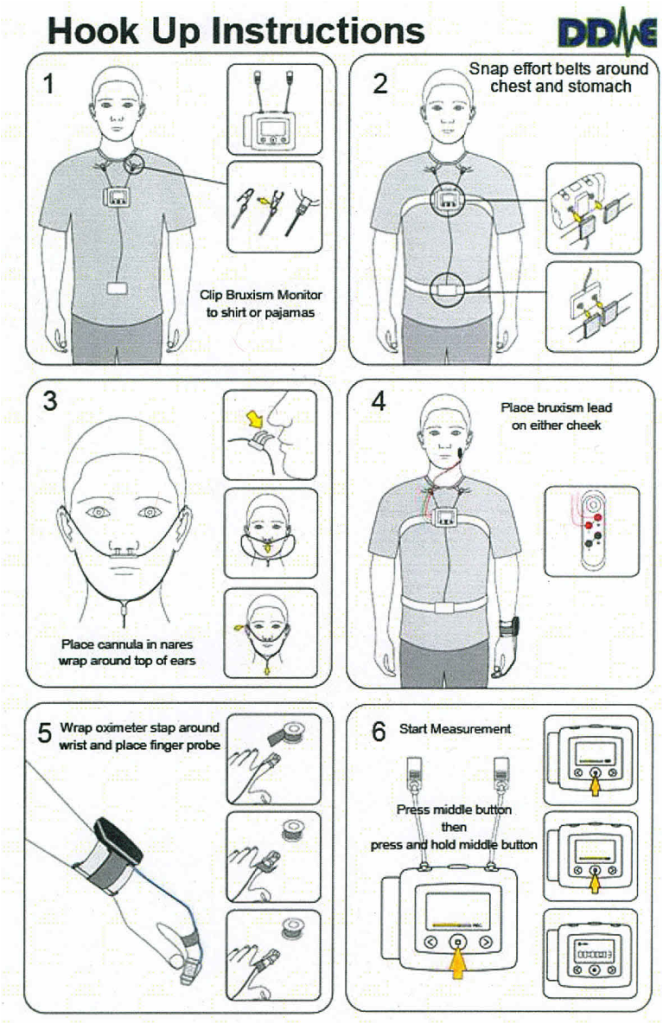
The NOX T-3 Sleep/Bruxism monitor and hook up instructions can be visualized below. It takes about five minutes for patients to hook themself up and is surprisingly comfortable to wear. The components are very small and do little to interfere with normal sleep position or comfort. (I personally hooked it up and wore it for a sleep study on myself. I am a light sleeper and had no problems hooking it up or having a normal night’s sleep.)
For detailed hookup instructions, click on the above image.
Treatment:
Dental treatment or management of any of these disorders will involve some type of oral appliance. The type or design of the appliance will depend upon the type of disorder(s) (sleep apnea vs. snoring vs. nocturnal parafunction), the severity of the disorder(s), and factors causing or contributing to the disorder(s). Therefore, identifying all three of these issues is critical.
For example, often times, nocturnal parafunction is affected by biomechanical disharmony as well as sleep factors (see “Dental Biomechanical Harmony – the Key to Predictable Dental Comfort, Health, and Esthetics” and “Biomechanical Disharmony – Problems, Evaluation, and Treatment”). When this is the case, correcting the biomechanical disharmony should be part of the treatment, along with a properly designed night guard appliance. As another example, obstructive sleep apnea and snoring are often worse when patients are overweight. Therefore, if weight is a factor, weight management should be a part of treatment along with a dental airway-opening appliance.
An important note regarding dental appliance use is that it is not always the most appropriate treatment for patients with obstructive sleep apnea. CPAP (Continuous Positive Airway Pressure) machines are still the preferred treatment for many sleep apnea sufferers, especially those with severe apnea. However, for many patients, the use of CPAP machines is not practical or possible – for either some nights (such as during travel) or any nights. Therefore, for many patients a dental airway-opening appliance is indicated for either occasional or every night use.
Finally, regardless of the treatment for sleep apnea, it is critical that a follow-up sleep study (home or sleep center) be performed to confirm that treatment is working. The cessation of snoring or simply feeling better are good signs, but do not confirm that the sleep apnea has been eliminated or reduced to a safe level. Confirmation is only possible with a follow up sleep study.
A Simple Test:
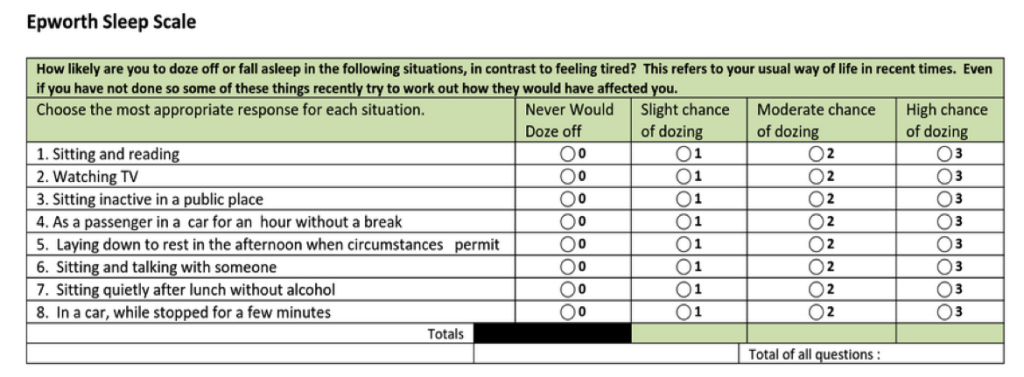
In closing, if you even suspect that you might be suffering from sleep apnea, we encourage you to take the simple screening test below. If you score a “10” or higher, it is recommended that you have a sleep study performed, either at home or at a sleep center. The lives you affect may not only be your own, but those of all who love you.
Click on the image below for printable PDF version.